TOTAL KNEE REPLACEMENT
Your consultant has advised you to have a joint replacement. There is no need to worry about this because over 75,000 knee replacements are carried out in the UK every year. Knee replacements improve the quality of life for patients more than almost any other operation carried out. They are second only to heart bypass surgery in life quality improvements.
Despite being successful, knee replacements are major operations. With such surgery comes a multitude of questions and hopefully most of these will be answered below.
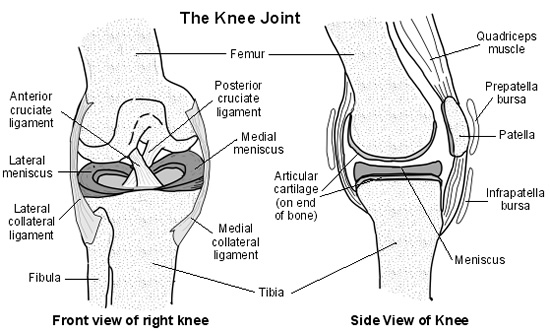
You may need a knee replacement because your knee joint is badly damaged, either by wear and tear or injury. The knee is a hinge joint, made up of the thigh bone (femur) which sits on the lower leg bone (tibia).
Joint replacement is a very successful operation and 95% of patients who have this operation (19 out of 20 people) report significant improvement after surgery
If part of your bone has become thin, we may need to replace the loss with a bone graft. The source of this bone graft is usually bone from someone else, removed when they had a hip replacement or donated after death.
A cut will be made down the front of your knee joint. The damaged ends of both bones will be removed and replaced by the artificial joint. This artificial joint consists of a curved metal piece, which replaces the bottom part of the thigh bone and a flat plate of metal, which replaces the top part of the tibia. A plastic plate is fitted in the middle to help your joint move more easily; these parts may or may not be cemented in place, depending on your age, the wear and tear on your joint and the type of joint being used.
The major benefit is a reduction in pain. You will usually notice the benefits immediately. You may also have an increase in movement and improved ability to carry out your day to day activities. However, it is important to realise that an artificial knee is not as good as a natural knee and will have some limitations.
With all surgery there is a risk of complications. If your knee is badly damaged or worn, or you have other medical conditions, then the risk of complication could be higher. Other possible complications include:
- Minor chest or wound infection – this sometimes occurs and you may require antibiotics and, in the case of deep wound infection, further surgery may be needed.
- Blood clots – surgery to the leg can sometimes cause a blood clot to form in the veins. To help prevent this you will be given injections whilst in hospital and taught how to administer these to yourself for 4 weeks after your surgery.
- Stiffness – sometimes the knee becomes very stiff and it may be necessary to bring you back into hospital to bend your knee under anaesthetic. The need for this intervention is greatly reduced if you follow the post op physio advice and practice your exercises on a regular basis.
- Loosening – although rare, the new knee can become loose and will require further investigation/surgery.
- Nerve damage - the nerves around your knee can be damaged at the time of surgery. If this occurs it may require further investigation
Up to 15% of patients can experience long term problems with pain following total knee replacement surgery, despite having a well functioning knee.
Please discuss these issues with the medical team if you would like further information.
It is essential that you are in the best of health possible to reduce the risks from having an anaesthetic and to help with your recovery. It is very important that you prepare yourself for surgery as best you can. If you are unwell at any stage prior to surgery, call your Consultants secretary to discuss further, using the Hospital phone number.
It is essential that you are in the best of health possible to reduce the risks from having an anaesthetic and to help with your recovery. It is very important that you prepare yourself for surgery as best you can. If you are unwell at any stage prior to surgery, call your Consultants secretary to discuss further, using the Hospital phone number.
Weight and Diet
If you are overweight you will put more strain on your new knee you are advised to lose some weight before your surgery. Excess weight can also make you more likely to have anaesthetic problems. If you are underweight or have a poor appetite, it is important to make the best of what you do eat. Dietary advice and further information can be obtained from your local GP practice.
Body Mass Index
Body Mass Index (BMI) is a measure used to evaluate body weight relative to a person's height. BMI is used to find out if a person is underweight, normal weight, overweight or obese. If your BMI is above 35 you will need an anaesthetic assessment (above 30 if you have any other medical problems).
Smoking
It is recommended that, if possible, you cut down on your smoking immediately. Ideally you should not smoke for a week before your operation and not all whilst in hospital.
About two weeks before your operation you will be asked to attend a pre-assessment clinic, where you will undergo routine tests to assess the state of your health before surgery and to confirm that you are healthy enough to have the operation.
You will have an ECG, which is a tracing of your heart and, if necessary, a new x-ray of your knee.
At the clinic you will be seen by a nurse who will check your blood pressure, pulse and weight. Some blood samples will be taken to ensure that all your blood levels are acceptable.
You will also be asked for a specimen of urine. This is routine to make sure you do not have any water infections prior to surgery.
Fasting
You will be asked not to eat or drink anything for 6-12 hours before your operation. This will let your stomach empty to prevent you from vomiting during your operation.
Timing of the Operation
The approximate timing of your operation is arranged the day before surgery. Once the operating list order has been confirmed by the surgeon and anaesthetist, you will be informed of an estimated time of your operation. This may be subject to change at short notice.
Preparation for Going To Theatre
You will be asked to remove all contact lenses, jewellery, watches, make-up and nail varnish. Wedding rings can be covered with tape if they will not come off. (Ideally you should not bring jewellery into hospital with you). You will be asked to take a bath or shower. Antiseptic skin wash will be provided for you to wash with. The operation site will not be shaved on the ward. If it is necessary, we will shave it in the operating theatre. Dentures will have to be removed once you are called to go to theatre.
Pre-Medication
You may be given a sedative injection or tablets about 1 hour before the operation. This will relax you and may make you sleepy. Once you have had your ‘pre-med' you must stay in bed. You should call for a nurse if you need assistance.
Transfer to Theatre
A ward nurse and a theatre porter will take you on a trolley to the operating suite. You will be wearing a cotton gown. There will be several checks on your details on the way to the anaesthetic room where your anaesthetic will begin.
Having an Anaesthetic
You will be reviewed by the anaesthetist on the ward prior to being taken to theatre. The anaesthetist will discuss the anaesthetic options available to you, this will be either general anaesthetic or spinal (epidural) anaesthetic. Once the decision on which anaesthetic will most suit you, the anaesthetist will either help you to sleep with a general anaesthetic via an injection in the back of your hand, or perform the spinal (epidural) anaesthetic which will numb you from the waist down. The operation is then performed.
After the operation, you are taken on a bed to the recovery ward for about half an hour. Once you are fully recovered, you will be transferred back to the ward on a bed.
Coming Round After The Anaesthetic
Although you will be conscious a minute or two after the operation ends, you are unlikely to remember anything until you are back in your bed on the ward.
You may wake up with an oxygen mask on your face. This is to help you come round from the anaesthetic.
You will have a plastic tube in your arm to give you a drip, which will ensure you remain well hydrated.
You will have a fine plastic drainage tube coming out of the skin near the wound, connected to a container which will measure any blood loss after the operation. If an adequate amount of blood is collected within a certain time frame, you will be given back your own blood, via a drip. This should greatly reduce the need for you to have a blood transfusion post op.
Warning After a General Anaesthetic
The drugs that we give for a general anaesthetic will make you clumsy, slow and forgetful for about 24 hours. This happens even if you feel quite all right.
For 24 hours after your general anaesthetic: Do not make any important decisions.
Will It Hurt?
The wound may be painful. You will be given injections or tablets to control this. Ask for more if the pain is unpleasant.
Drinking and Eating
You should be able to drink within an hour or two of the operation provided you are not feeling sick. The next day you will be able to manage normal food, and you must focus on drinking plenty of fluids to ensure you remain hydrated.
Passing Urine
It is important that you pass urine and empty your bladder within 6-12 hours of the operation. You will need to use a bottle or a bedpan with help from the nurses at first. If you still cannot pass urine let the nurses know and steps will be taken to correct the problem. If necessary you may require a catheter.
Opening Bowels
It is quite normal for the bowels not to open for a day or so after an operation. You may need help with a bedpan at first. Later you will be able to walk to the toilet, but you may still need help. If you have not opened your bowels after 2 days and you feel uncomfortable, ask the nurses for a laxative.
Sleeping
You will be offered painkillers rather than sleeping pills to help you to sleep. If you cannot sleep despite the painkillers please let the nurses know.
Physiotherapy
Whilst in bed, you should help your circulation by continuously moving your ankles and legs. You will be helped out of bed, usually on the day after your operation. By the time you go home you will be walking with the help of two crutches. If you have stairs at home, you will be taught how to climb and descend stairs before you are discharged. You will be informed of the amount of weight to put on the affected leg after the operation.
The Wound And Stitches
The wound will have a simple adhesive dressing over it. The nurses will remove your wound drain one day after your operation by pulling it out.
Your wound will be closed by either a continuous stitch under the skin or clips (similar to staples). The continuous stitch is dissolvable and will not need to be removed, or staples will be removed at 14 days post op. These will be removed by either your practice nurse or the district nurses. Removal of stitches and wound monitoring will be organised prior to your discharge from hospital.
Washing
Wash around the dressing for the first ten days. You can wash the wound area as soon as the dressing has been removed. Soap and warm tap water are entirely adequate. Salted water is not necessary. You can shower as often as you like.
What About Informing my Relatives and Contacts?
With your permission, the nurses will keep your relatives and contacts up to date with your progress. However, please help minimise the number of phone calls to the ward. Organise a few key people who can ring and distribute news of your progress.
How Long In Hospital?
Depending on your recovery you will usually be in hospital for 4-6 days following your operation. Occasionally this may be longer. You may go home when you can walk safely with crutches or sticks. You will be given an appointment to visit your consultant in the Orthopaedic Outpatient Department six weeks after your operation. The physiotherapist will make arrangements for you to attend the physiotherapy department as an out-patient.
Clothes
Please bring in loose fitting clothes to wear on the ward. This is because they are easier to get on and off.
Transport
When you are fit for discharge from hospital, you can go home in a car. You will be taught how to get in and out of a car in a safe manner
Sick Notes
Please ask the nurses if you require sick notes, certificates etc.
Driving
You must not drive for at least six weeks after you leave hospital. You will not be able to carry out a full emergency stop procedure during this post op period. The majority of insurance companies will not insure drivers during this post op phase - it is advisable to confirm with your insurance company. You should confirm your ability to return to driving at your six week post-op out-patient check up.
Work
This depends on your job. If you have a job which is not particularly physical you may be able to return to work at approximately 8 weeks post op, most people will return to work at the 12 week post op stage.
General Recovery
Your knee will continue to improve over a six to twelve month period.
Total knee replacement surgery is a major undertaking. However, we believe that you will be much better off with a new knee joint.
If you have any problems or queries, please ask the nurses or doctors.
It is important that you keep as fit and active as you can, as this will help your recovery after the operation. Gentle exercises will help you remain fit as possible and may also help to reduce some of your joint pain whilst you are waiting for your operation.
Exercise is most helpful when practiced regularly. You should therefore try to make time every day to practice, even if it is only for five minutes. You can even do some exercises whilst watching TV.
Some Helpful Exercises:
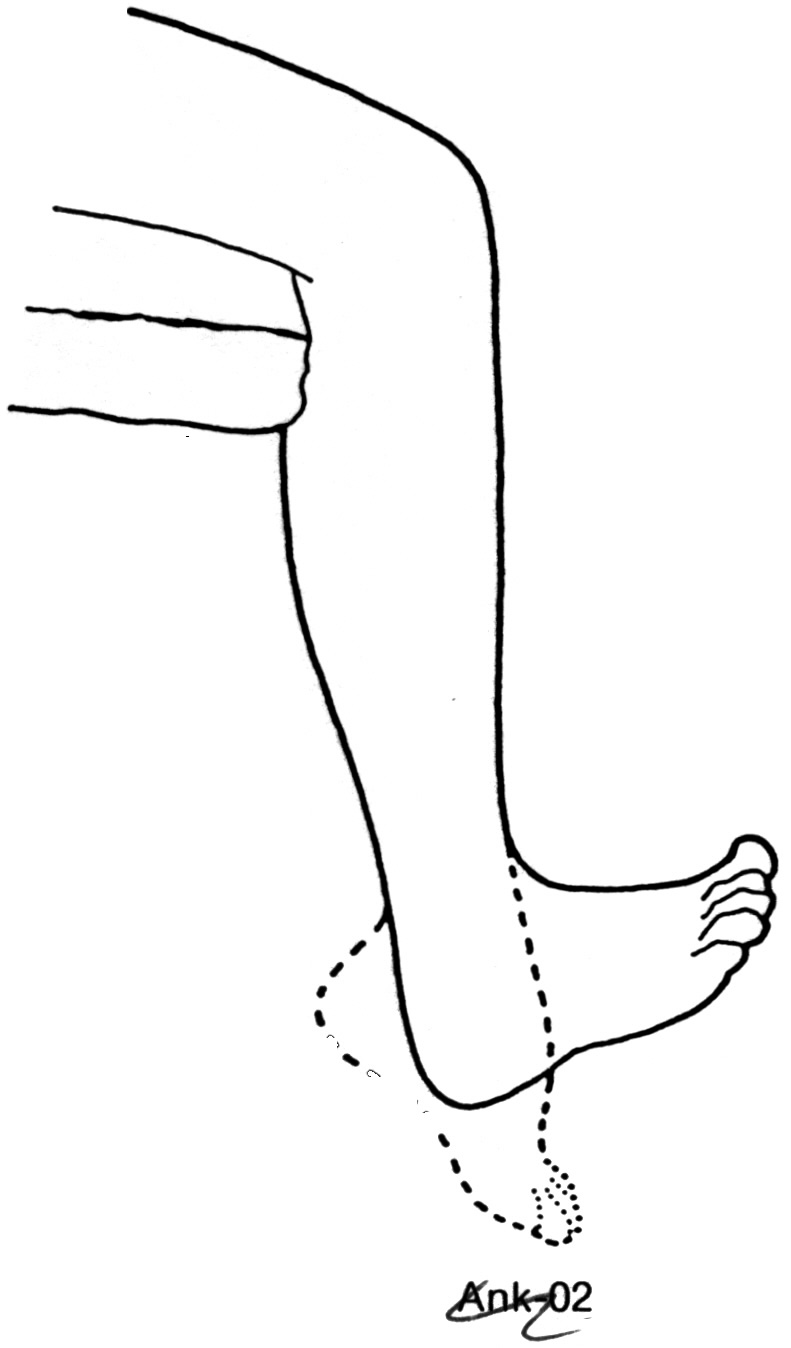
Foot Paddling - Sitting in a chair, slowly point your whole foot away from you towards the floor and then move your foot upwards. You can practice this with both feet.
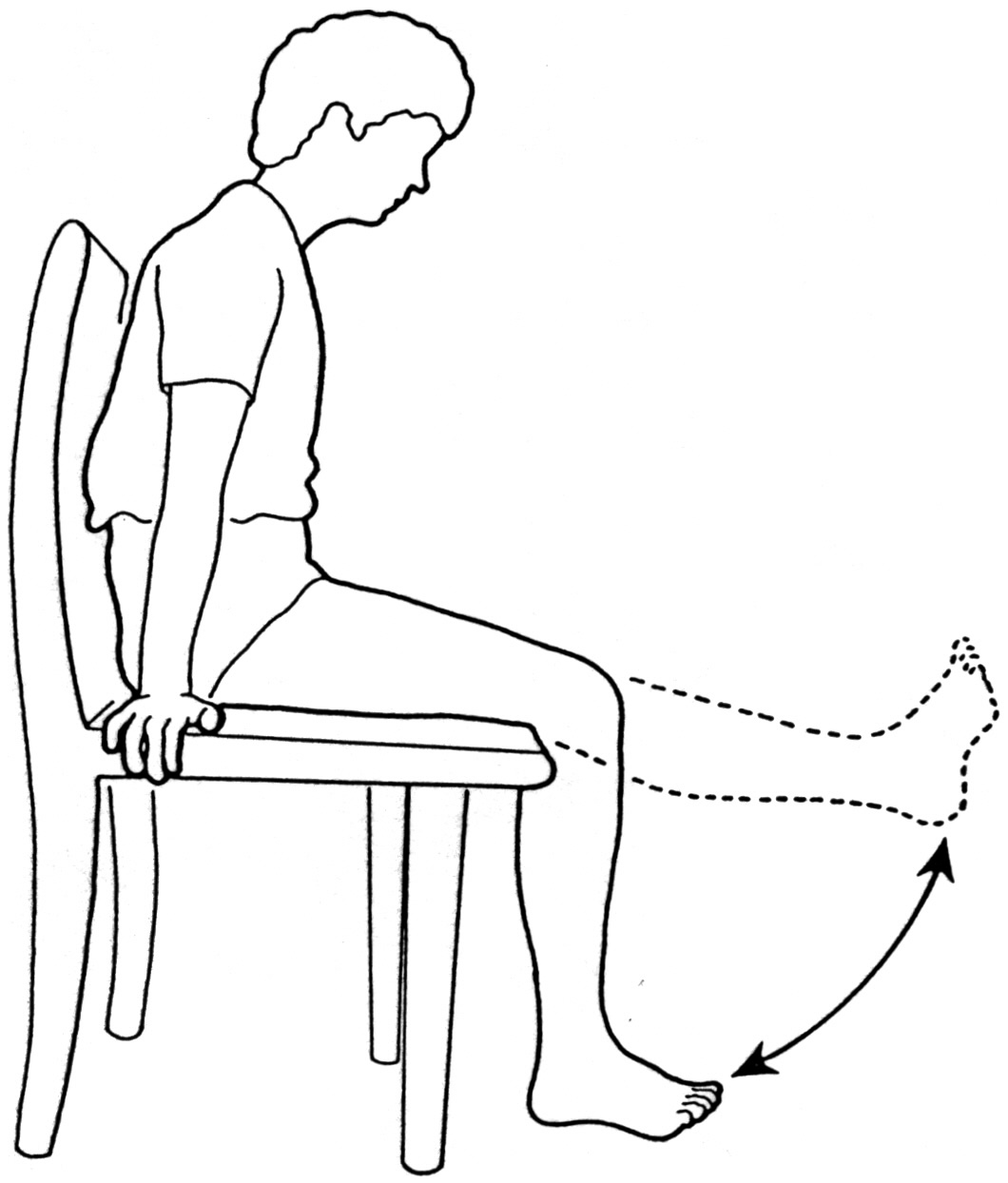
Leg Raises - Sitting in a chair, raise your foot off the ground to straighten your knee and then lower the foot back down to the floor again. You can practice this with both legs.
Arm Exercises - Raise both arms above your head and try to clap your hands, and then lower them down by your side.
Walking - Walking is one of the best ways of exercising, as it helps to keep your joints moving and strong and is also good for your heart and lungs. Try and walk a short distance every day, as far as your pain allows you to go. You may need to use a stick, frame or crutches to help you walk – don't let this stop you practising.
You may be afraid to exercise because of the pain you have. Some people find having a warm bath or shower before they practice their exercises helps to lessen some of the pain, as the warmth of the water is very relaxing. Swimming itself is an excellent form of exercise, as you will be able to move and strengthen your joints and benefit your heart and lungs, whilst the warmth of the water helps to relieve your pain.
Special note – It is advisable to consult a doctor, nurse or physiotherapist before attempting any new form of exercise.